I had the unique opportunity at the University of Utah Hospital to photograph the first kidney transplant into an HIV positive patient in Utah last week. This was a revelation to me as I remember distinctly when HIV came onto the scene in the 1980s. Seeing it go from a deadly diagnosis to a chronic disease does my heart so much good not only for the people impacted by the HIV virus, but also because this is a remarkable achievement made possibly only through public investment in science and research to the National Institutes of Health.
Note: There are graphic surgical images and animated gifs below.
While I’ve photographed neurosurgeries before, this was my first experience seeing an organ transplant. The surgery on the surface, is relatively straight forward. A donor patient is identified for the recipient, rigorously tissue typed for compatibility, then both patients are scheduled and prepped for surgery simultaneously. The plan, carried out without a hitch, was to bring both patients into nearby operating suites, remove the kidney from the donor, prepare the kidney for transport and implantation, walk the donor kidney to the adjacent operating suite and then implant and close.
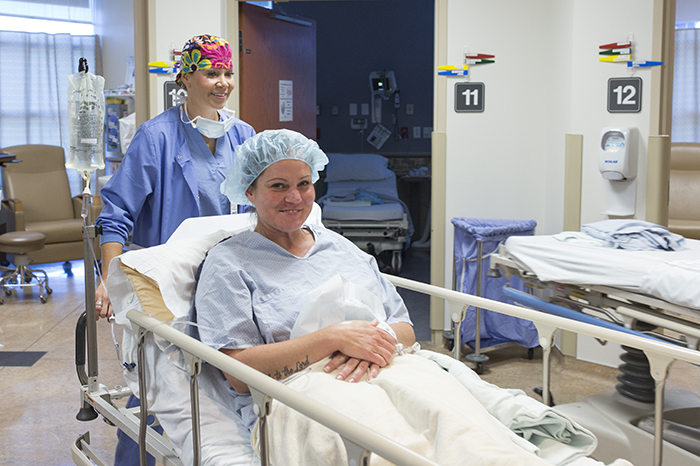
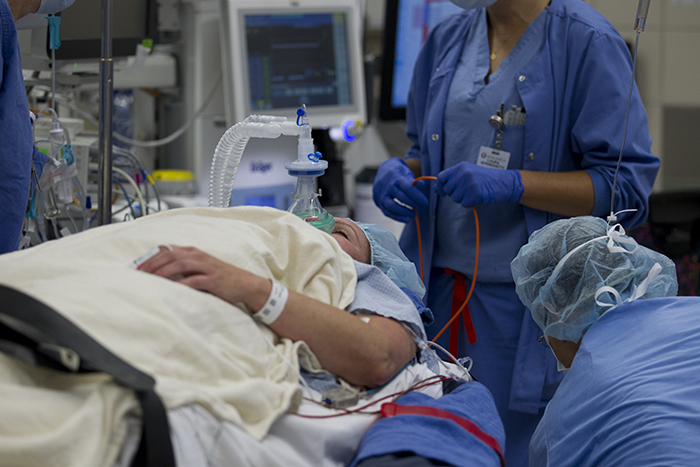
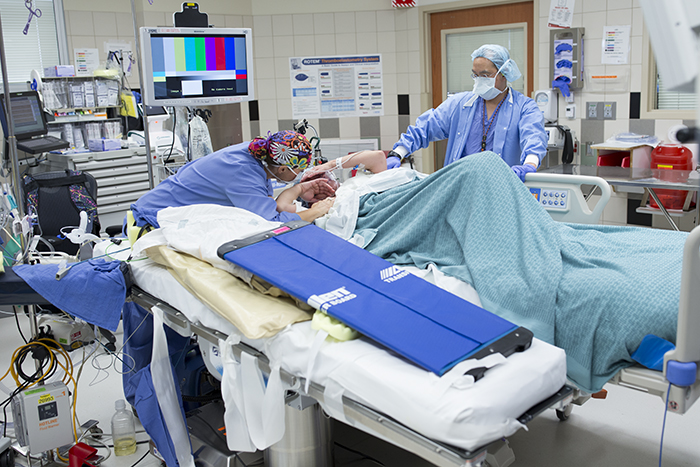
Patients in each operating suite are wheeled into the operating rooms at the same time and put under general anesthesia.
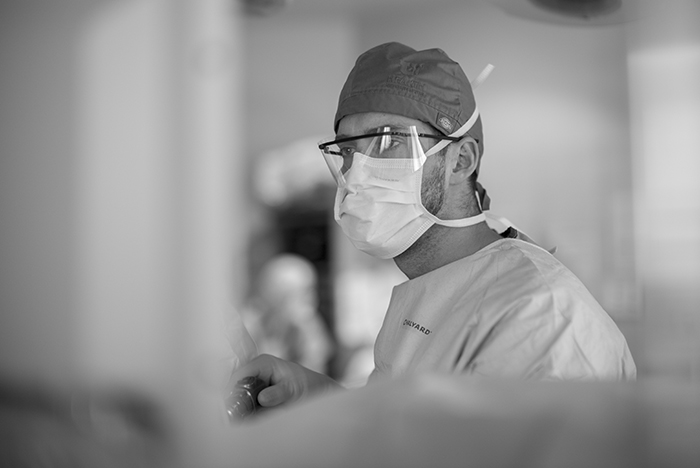
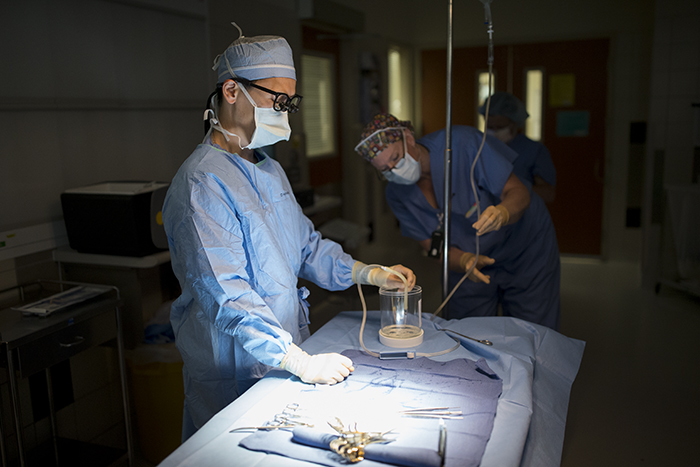
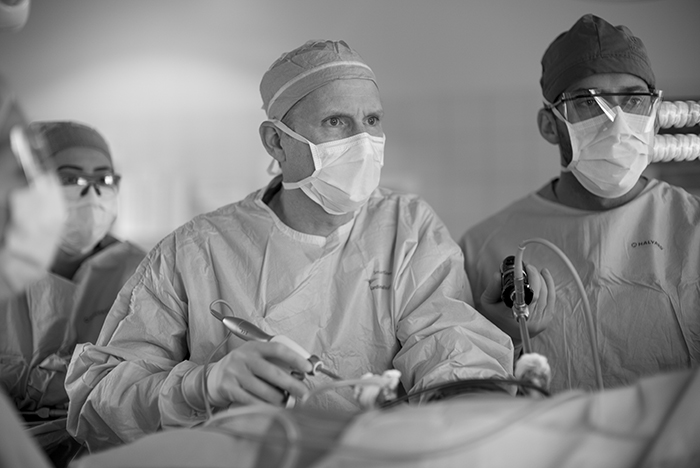
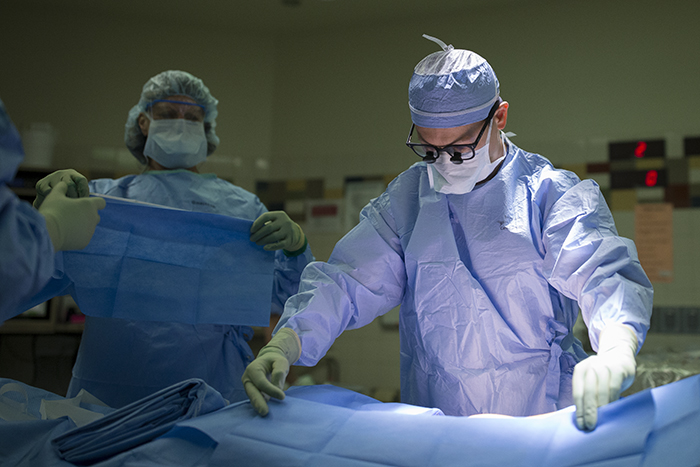
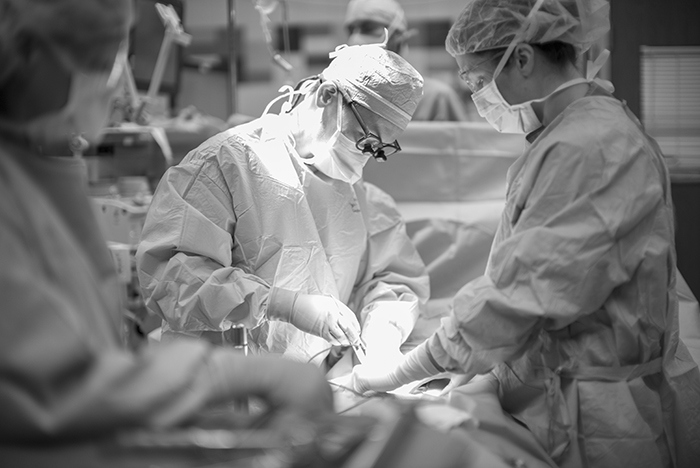
While the operating room staff and anesthesiologists prep the patients, the surgeons Robin Kim and Paul Campsen scrub in with newer protocols than I remember when I worked in operating rooms about 17 years ago.
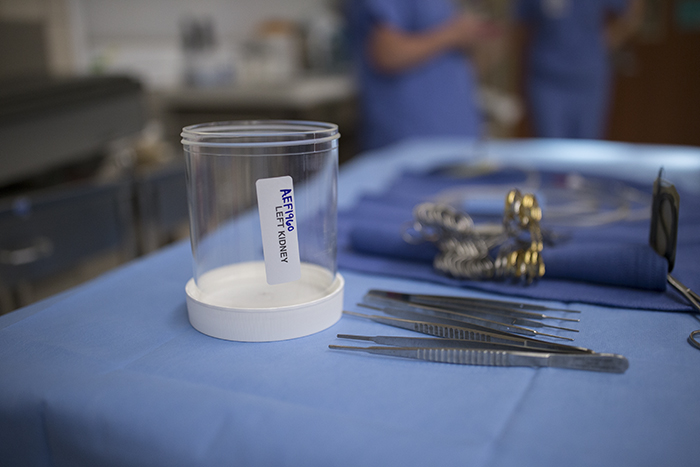
One of the remarkable things about being able to get out of my visual neuroscience laboratory a couple times a year and work as a photojournalist is being able to get an insight into the specialized knowledge involved in various jobs that we do not normally get an insight into. People tend to take for granted all of the incredibly precise knowledge that goes into all of the jobs around us from garbage collectors to rocket scientists. So, just watching the operating room staff prepare for the kidney transplants was incredibly interesting. Every instrument has its place and there is protocol for everything. Precise movements and instruments dictated by the type of surgery, the surgical approach decided upon and sterile technique coalesce to form a precise dance that the technical staff, nursing staff and physicians go through.
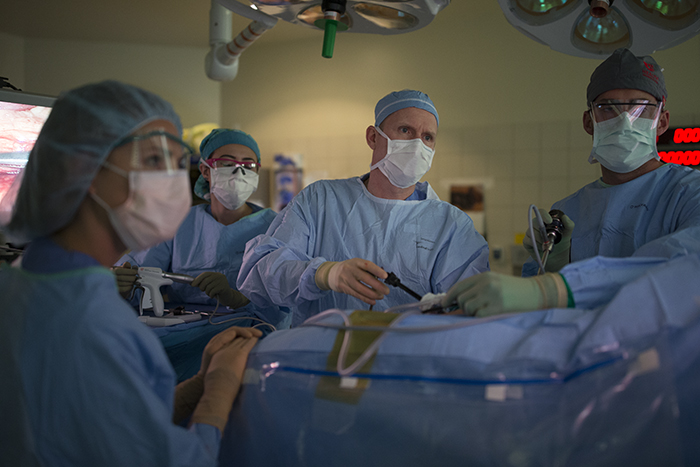
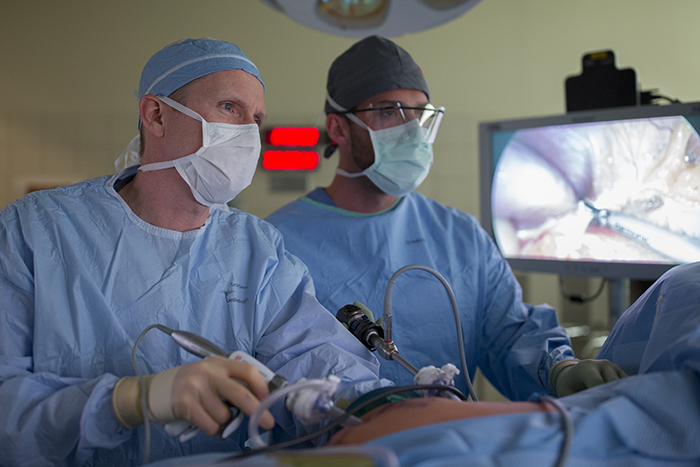
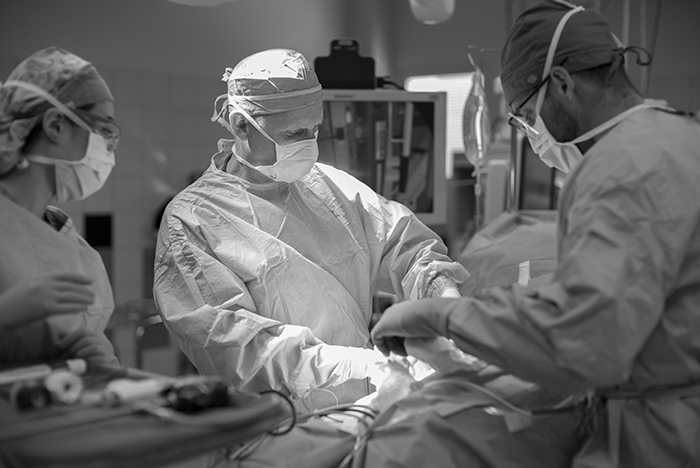
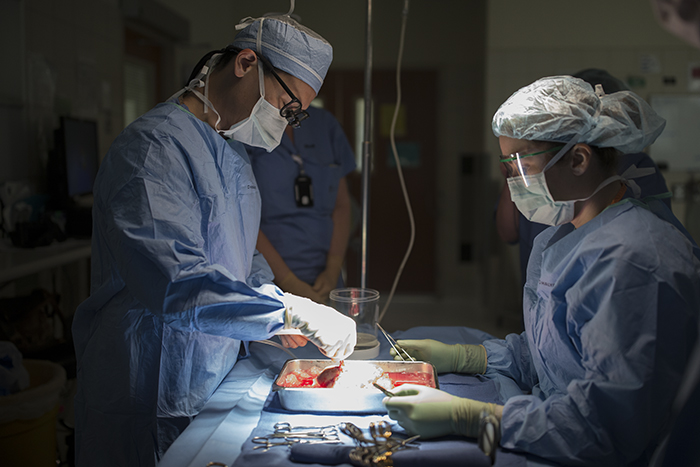
For the donor kidney removal, both surgeons work together in the same operating room with one, Robin Kim in this case preparing to receive the kidney.
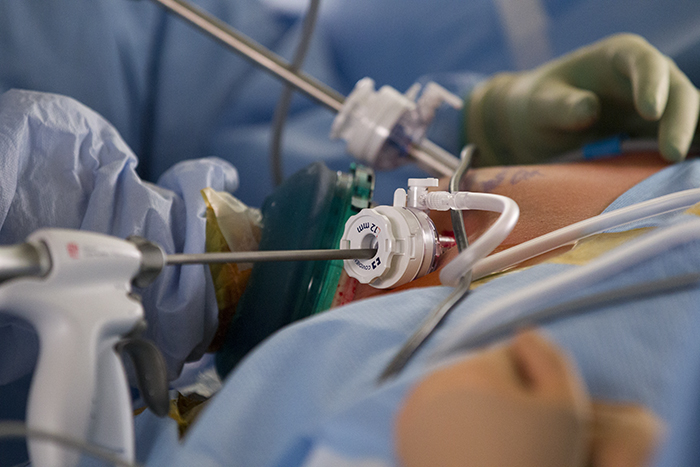
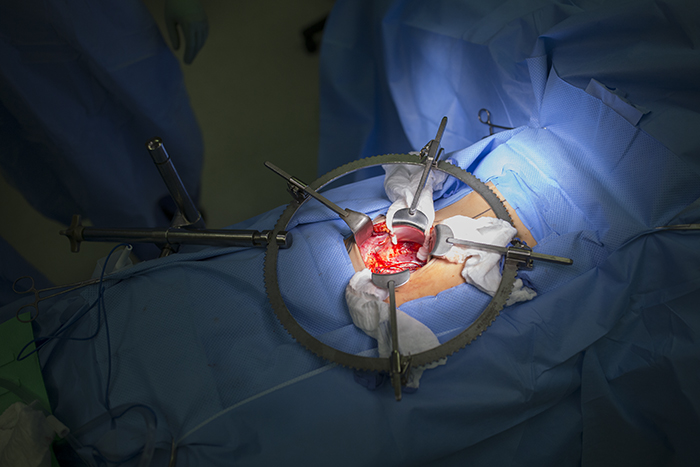
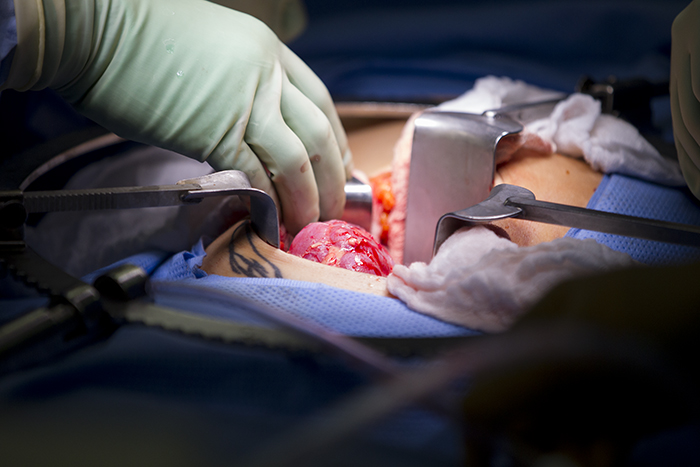
The surgeon removing the kidney, Paul Campsen assisted by physicians assistants and nursing staff installs a port to reach into the body of the donor with one hand to position and stabilize tissues, while manipulating laparoscopic instruments with the other hand to carefully remove the kidney from the donor.
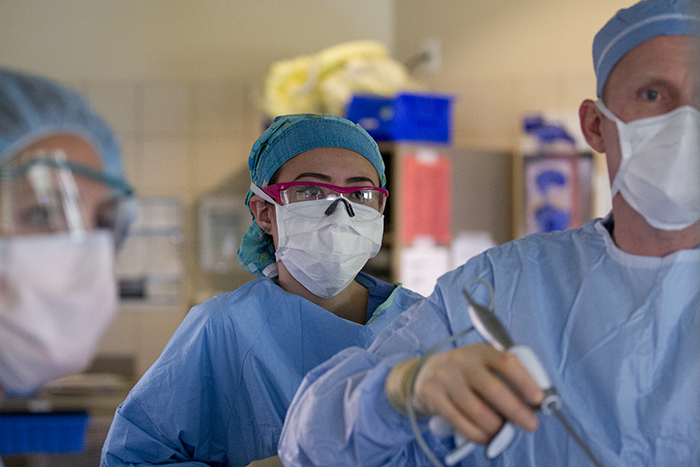
Each person in the operating room team has a specific role, including the anesthesiologists and the nurse anesthetists who constantly maintain vigilance of the patients vitals and anesthesia induction and maintenance.
Donor nephrectomies or removal of the entire kidney along with a section of the ureter and the blood vessels that both supply the kidney with oxygen and nutrients and drain the kidney of waste and C02 is a complex procedure. The laparoscopic approach is done with cameras on wands that are passed through small holes in the body wall. The smaller the incisions, the better the surgical outcomes, with shorter a hospital stays and fewer post-operative complications.
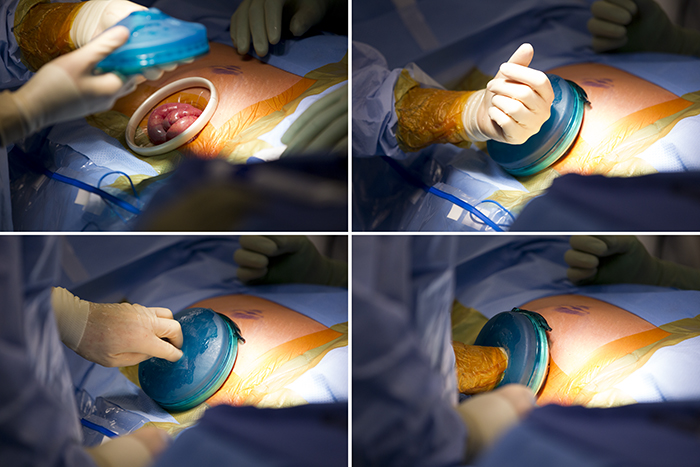
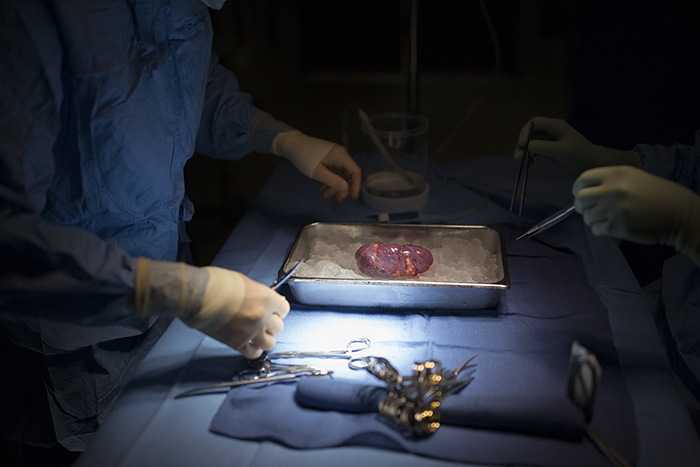
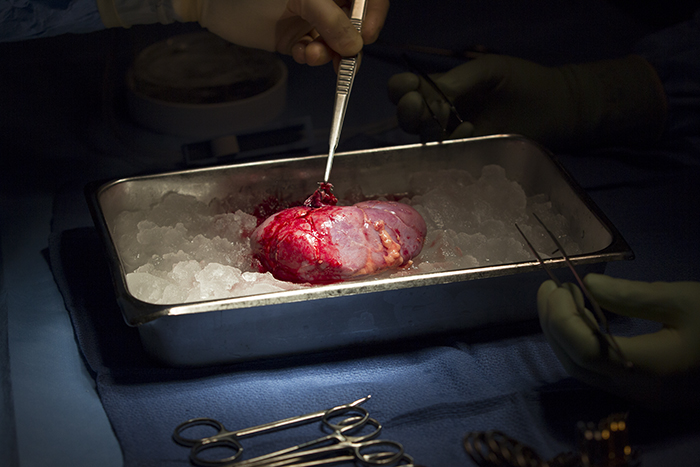
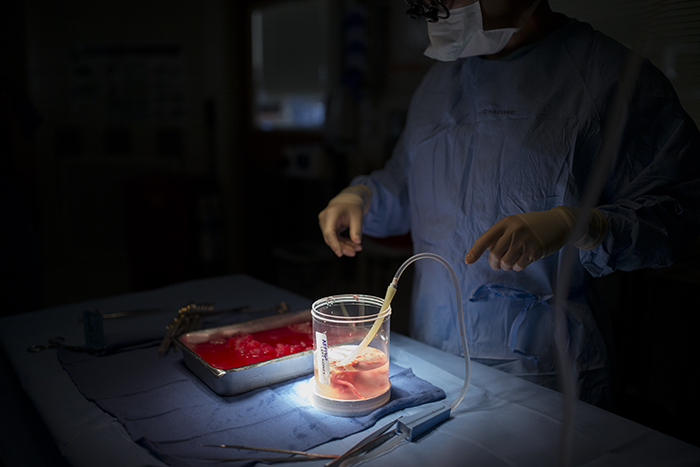
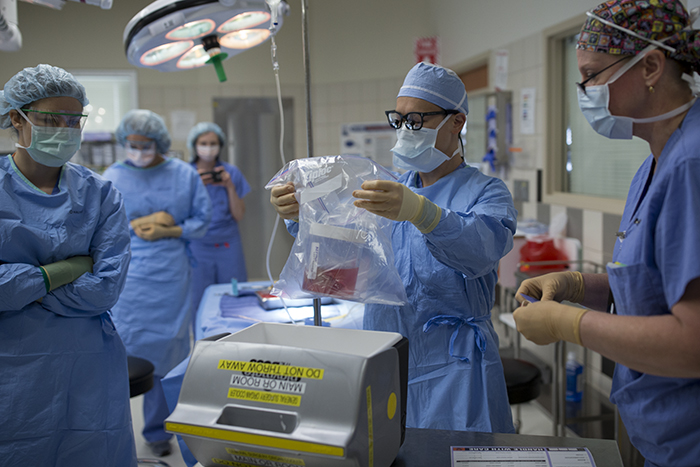
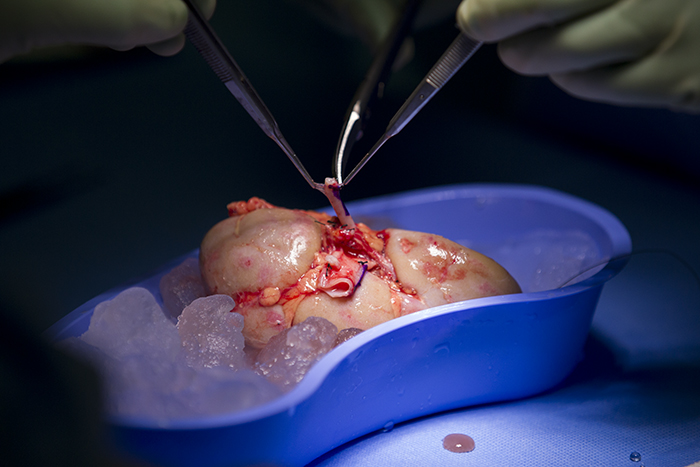
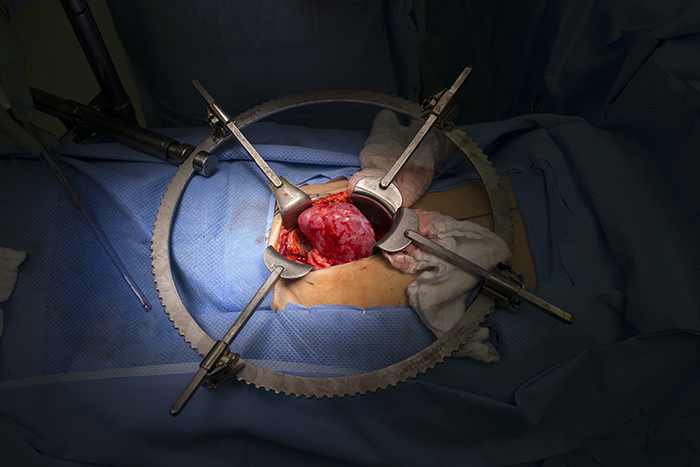
Once Dr. Campsen removes the kidney, Dr. Kim goes to work processing the kidney, removing the blood and flushing it with an organ preservative. It is truly remarkable to watch the bright red kidney grow pale as it is packed on ice while the blood leaves it, to be replaced by nutrients and preservatives for the short journey from the donor to the recipient.
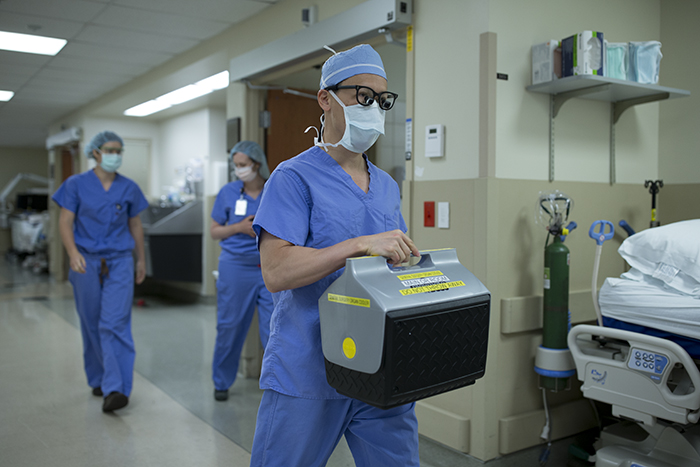
At this point Dr. Campsen begins the process of closing the donor patient surgical site and Dr. Kim takes the kidney from the donor operating room, places it into a cooler and walks it down the hall to the recipient patient’s operating room. This part of the journey is simple, but profound as a living organ physically travels from person to person through a physical space.
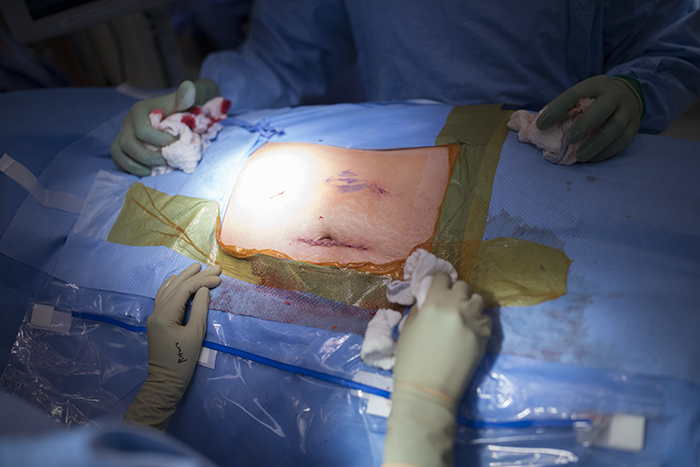
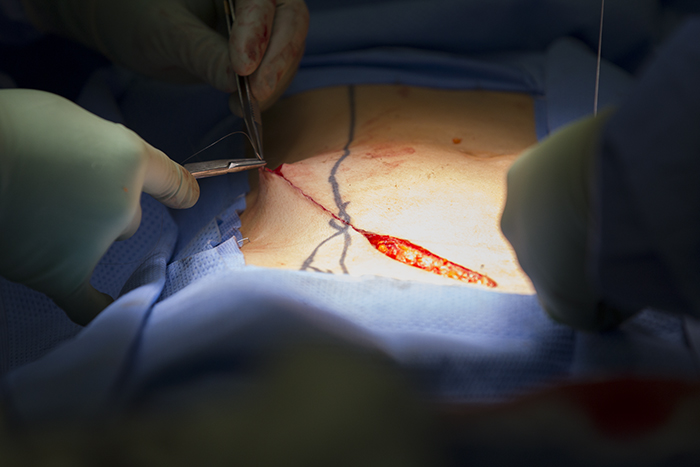
While Dr. Kim is preparing the kidney and taking it on its short journey down the hall, Dr. Campsen is closing the surgery for the donor. The scar from a kidney donors perspective is only about a six inch long line. After the patient surgical site is closed and the patient comes out of anesthesia, Dr. Campsen goes to talk with the donors family and fill them in on the successful outcome.
At this point, Dr. Kim scrubs in again and begins the process of placing the kidney into the recipient.
The thing that surprised me with this part of the surgery was that the kidney recipients original kidneys remained, so the donated kidney will become a third kidney that assists the first two failing kidneys.
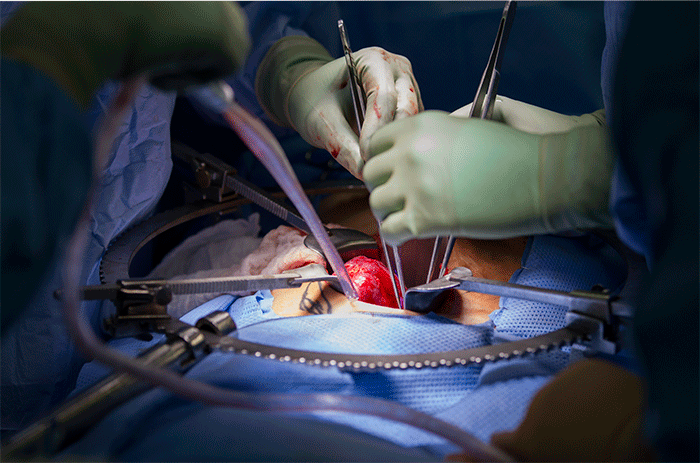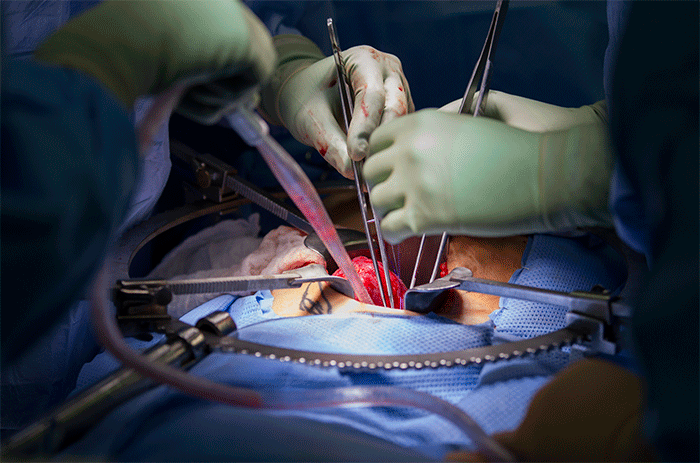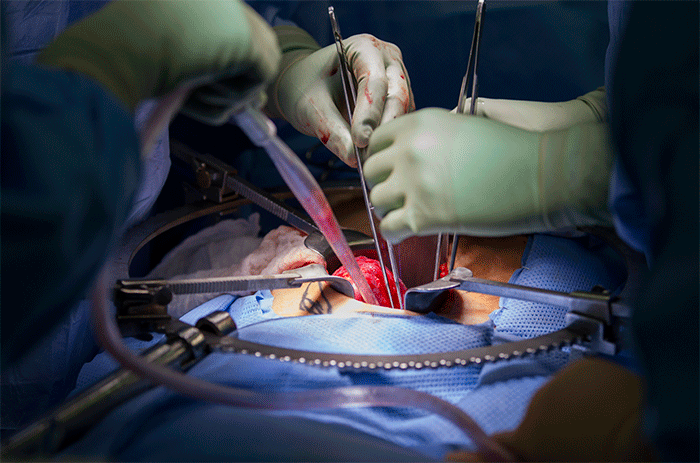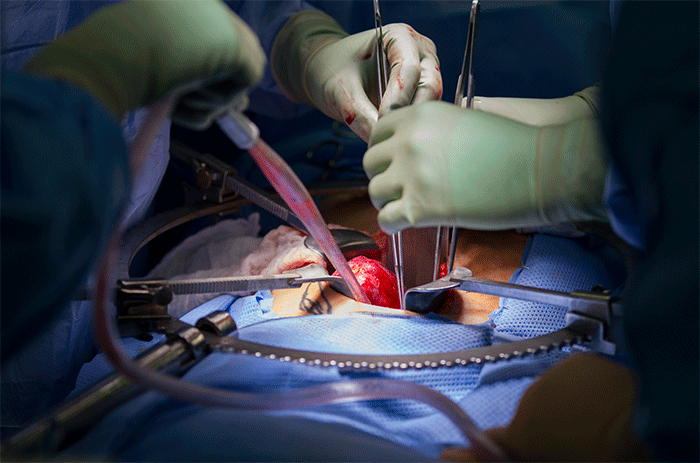
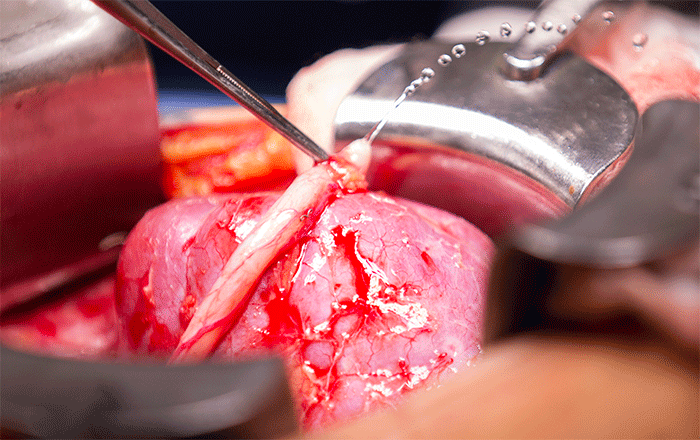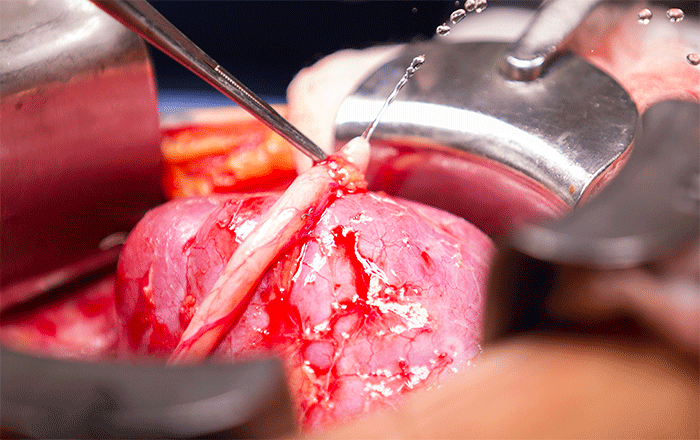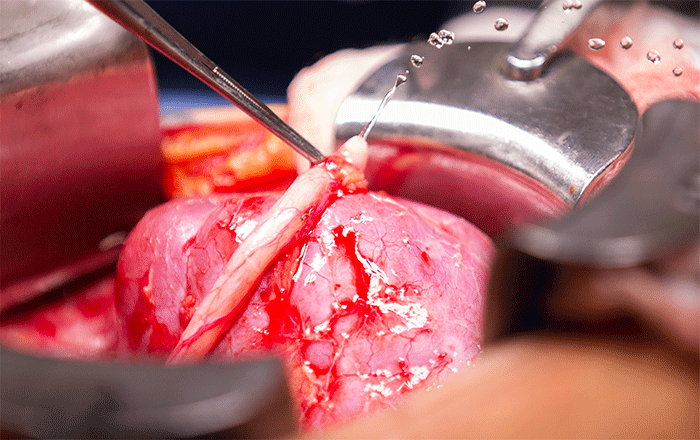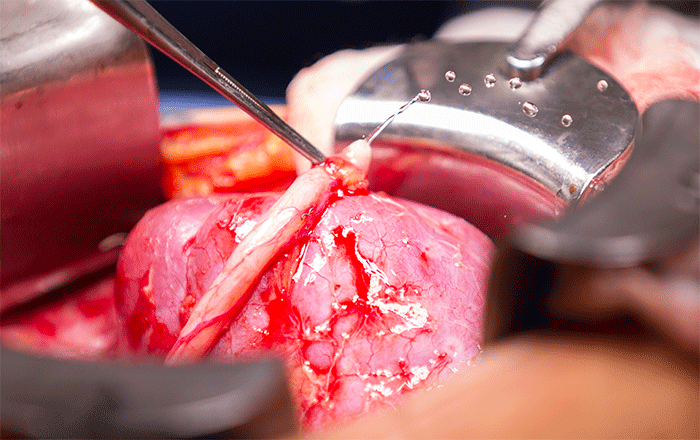
The procedure is to connect the renal veins, followed by the renal artery and then the ureter to the bladder. It was truly inspiring to see the organ grow bright pink again and flush with color once the blood supply was connected back.
The real tests comes after the blood supply is connected back up and the kidney begins to function again. I wanted to specifically capture this moment as seeing urine start spraying out of the ureter as the kidney function starts back up was a phenomenal experience.
I do have to say that watching Dr. Kim reconnect everything was inspiring. I am used to micro-surgery and taking things apart underneath microscopes for my experiments, but to watch a surgeon put it all back together again complete with precise, sub-dermal sutures while truly healing by giving the kidney recipient a new lease on life was humbling.
4 hours after we began this morning, we were done. After closing, Dr. Kim went to talk with the kidney recipients family while the nurse anesthetist and nursing staff helped wake the patient from anesthesia.
My thanks to Drs. Paul Campsen (@JeffCampsenMD) and Robin Kim (@RobinKimMD), the departments of surgery, organ transplant, anesthesiology and nursing for making this photo-essay possible. Also, many thanks to Libby Mitchell (@LibbyMitchellUT) and Heather Thiesset (@HeatherTSA) for working to make the logistics happen.













Thank you for keeping me hopeful! Wonderful work documenting this procedure. My search for a donor continues, but it great to see this working out for someone. #DonorsAreHeros
Thank you, and my very best wishes for you to find a donor soon Patrick.
Stunning work, Bryan! Wow.
Thank you Virginia.
Fascinating, Bryan! What a great gift in so many ways. Thank you for sharing.
Thank you Linda. It was a wonderful opportunity organized by Libby Mitchell.
Amazing photos and thoughtful insights. Thank you so much for sharing!
Thank you Kathy. The best part of it was the incredibly good vibe from all of the people who were involved. The feeling from literally every person on the team was one of compassion.
I think everyone else has already taken the adjectives I would have used to describe your series of photos and the commentary that accompanies them Bryan. Fascinating is probably the most descriptive one for me. The images are excellent and the commentary describing the procedures flows like a photojournalist telling a story with images and text. Very well done.
Thank you Bill.